The Autonomic Nervous System
The rhythmic discharge of the SA node is principally responsible for pacing the heartbeat. In the absence of extrinsic neural or hormonal influences, the SA node would discharge at a rate of about 100 impulses per minute. Heart rate and cardiac output, however, must vary in response to the needs of the body’s cells for oxygen and nutrients. The nervous system is one of the major influences on the heart that allows it to respond rapidly to the changing requirements of the body’s tissues.
The autonomic nervous system is the part of the central nervous system that controls involuntary activities such as digestion, respiration, and cardiac function. Autonomic nervous system control of the cardiovascular system originates in the medulla oblongata of the brain. Two specialized neural pathways-the parasympathetic and the sympathetic nervous systems-have direct influences on the heart. At any given time, the effect of the nervous system on the heart is the net balance between the opposing actions of the sympathetic and parasympathetic systems.
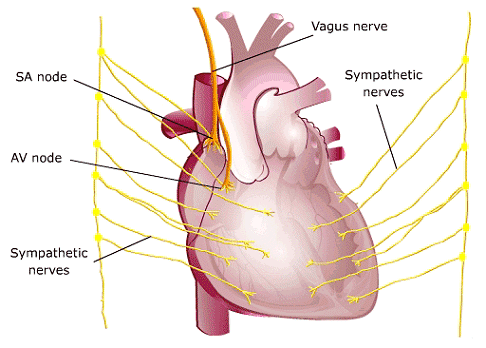
The Parasympathetic (Vagus) and Sympathetic
Systems Innervate the Heart
Artwork source:The Heart of Nuclear Cardiology, An Interactive Primer; © 2002 Bristol-Myers Squibb Imaging. Inc.
Tuning the Heart Rate
- Sympathetic stimulation increases the heart rate, accelerates the spread of excitation through the cardiac conduction system and increases myocardial contractility.
During exercise, emotional excitement or many forms of disease, sympathetic control predominates, and cardiac function is increased. - Parasympathetic stimulation decreases the heart rate and slows the spread of excitation. During rest, sleep or emotional tranquility, parasympathetic control dominates, maintaining a resting heart rate of 65 to 75 beats per minute.
Cardiac Acceleration- the Sympathetic Pathway
In response to stress or exercise, the sympathetic nerves release the hormone norepinephrine. Norepinephrine increases the permeability of myocardial cells, including pacemaker cells and contractile tissue, to sodium and calcium. The increase in sodium permeability lowers the threshold potential of SA node cells, causing them to fire more rapidly. Increased sodium permeability in the AV node makes it easier for each fiber to excite the next, which decreases the conduction time from the atria to the ventricles. The effect of norepinephrine to increase the contractile strength of cardiac muscle is thought to be due to increased membrane permeability to calcium. Calcium ions play an important role in the contraction of myofibrils.
The effect of sympathetic stimulation is to increase the overall activity of the heart:
- The SA node discharge rate is increased
- The excitability of all portions of the heart is increased, reducing conduction time
- The contractile force of atrial and ventricular muscle is increased
Cardiac Deceleration-the Parasympathetic System
Parasympathetic nerves travel from the brain to the heart in the vagus nerve. Stimulation of the vagus nerves releases the neurotransmitter acetylcholine, which increases the permeability of cardiac cell membranes to potassium. This permits leakage of K+ ions to the outside, creating a state of hyperpolarity in which the cells are less easily excited. The effect of parasympathetic stimulation on heart rate and speed of conduction is, therefore, just the opposite of sympathetic stimulation:
- The firing rate of the SA node is decreased.
- The excitability of AV junctional tissue is lowered, slowing transmission of the pacemaker impulse to the ventricles.
The Baroreceptors
Baroreceptors are sensory nerve endings composed of intertwined fibers that are stimulated by changes in pressure or stretch. They are located in the aorta and in the internal branch of the carotid artery. When the walls of these arteries are distended by an increase in blood pressure, the baroreceptors are stimulated, and information is transmitted to the brain via the parasympathetic nervous system. The parasympathetic system then responds (via the vagus nerve) by increasing the release of acetylcholine at the SA node, thereby decreasing heart rate and cardiac output.
Conversely, when the baroreceptors sense a decrease in vessel wall tension-as occurs when you stand up quickly-the parasympathetic system is inhibited, and sympathetic control accelerates the heart rate. The baroreceptors also activate sympathetic nerves to the ventricular myocardium, increasing the force of contraction of the ventricles.