CARDIAC STRESS TESTING: Exercise Treadmill Test
Noninvasive cardiac procedures for the diagnosis of coronary artery disease include Electrocardiography, Radiography, Echocardiography, Nuclear Imaging and Positron Emission Tomography. Of all these modalities, the electrocardiogram (ECG) is the most widely used diagnostic modality in cardiology. In addition to providing important diagnostic information on cardiac rhythmic patterns, electrolyte imbalances, and cardiac drug toxicities, the ECG plays a major role in the diagnosis of CAD by differentiating infarction from ischemic processes.
Stress Electrocardiography or exercise testing is a useful and noninvasive technique for evaluating cases of suspected or known CAD. The procedure combines electrocardiography with a graded exercise test to detect stress-induced alterations in cardiac electrical patterns that might signify myocardial ischemia.
Indications and clinical value. Exercise testing is reasonably safe, easy to perform, and relatively inexpensive. This procedure also may establish the diagnosis of CAD in patients with chest pain when medical history, physical examination, resting ECG, and attempts at relieving pain with nitroglycerin have not confirmed the diagnosis.
For patients with known angina pectoris, exercise testing helps assess cardiovascular functional capacity, specifically the ability of coronary arteries to deliver adequate quantities of oxygenated blood to the myocardium under the demands of stress. Such testing can demonstrate the level of physical exertion a patient can safely perform without symptoms or ECG changes. Exercise tests also may help detect cardiac rhythm disturbances induced by exertion, so that appropriate measures can be taken to prevent them. Finally, periodic exercise testing is useful in evaluating an individual’s response to conditioning or recuperation programs.
For a discussion on an alternative to exercise, advance to pharmacological stress agents.
Contraindications and precautions.
Based on a patient’s past medical history or present complaints, a physician may decide that exercise testing should not be performed.
Absolute contraindications to stress testing include:
- Recent systemic or pulmonary embolus
- Acute thrombophlebitis in the lower extremities
- Significant aortic valvular stenosis
- Decompensated congestive heart failure
- Unstable ST-segment or T-wave ECG abnormalities/ evolving MI
- Previously undiagnosed complete heart block
- Systemic illness
- Refusal to give informed consent
Relative contraindications to exercise testing:
- Unstable angina
- Idiopathic hypertrophic subaortic stenosis (IHSS)
- Ventricular aneurysm
- Uncontrolled metabolic diseases such as diabetes, adrenal insufficiency, and renal failure
- Severe systemic or pulmonary hypertension
- Uncontrolled supraventricular rhythm disturbances
- Complete or second-degree heart block
Special considerations.
Certain conditions require special considerations or precautions prior to exercise testing. For example, ECG interpretation may be difficult or even impossible in the presence of conduction disturbances such as bundle branch block. Patients with peripheral vascular, neuromuscular, musculoskeletal, and arthritic disorders may be unable to perform on a treadmill or bicycle as well as those who do not suffer from such impairments. Similarly, patients with severe anemia, marked obesity, or pulmonary, renal, hepatic, or adrenal insufficiency may have great difficulty performing an exercise test. Patients with complete heart block may be unable to accelerate their heart rate adequately in response to exercise. Patients with fixed-rate pacemakers have similar difficulties. Pharmacological stress testing is an ideal method of establishing and/ or confirming CAD in these types of patients.
Rationale and procedure. Stress electrocardiography indirectly evaluates the adequacy of coronary blood flow under conditions of maximal oxygen demand. An individual who sustains maximal oxygen demand without demonstrating symptoms or ECG evidence of myocardial hypoxia is assumed to have essentially normal coronary circulation.
As myocardial oxygen consumption increases during exercise, a corresponding increase in coronary blood flow should occur. Since the extraction of oxygen by the myocardium is already maximal at rest, the increase in oxygen demand must be met primarily by an increase in coronary blood flow. An ECG recorded during exercise demonstrates the difference between oxygen demand (myocardial oxygen consumption) and oxygen supply (coronary blood flow), as manifested by characteristic ischemic ECG changes, even in the absence of chest pain.
Equipment. During stress electrocardiography, the patient may exercise in several ways. European physicians have traditionally used bicycle ergometers, while American cardiologists have favored treadmills.
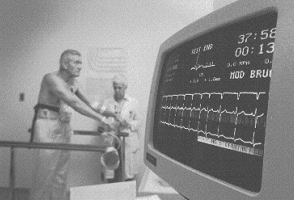
Preparation. The test is performed at least 2 to 4 hours after eating in order to avoid nausea and ECG changes caused by indigestion. Medications that may affect either the response to or the interpretation of the test may be discontinued from 1 hour to 2 weeks prior to the exercise, at the discretion of the referring physician. The patient is instructed to wear comfortable clothing and low-heeled shoes. Prior to the test, the patient must sign an informed consent form.
Monitoring.
Exercise testing should be done only under the direct supervision of a trained physician, with continuous ECG monitoring and periodic blood pressure determinations. The 12-lead ECG is routinely recorded in both the supine, sitting and standing positions prior to exercise. A pre-stress tracing with the patient hyperventilating a few seconds is optional. A standard 12-lead may also be recorded, using true arm and leg leads. During stress, one tracing is recorded two minutes into each stage of exercise. The patient is continuously monitored 5 minutes into the Recovery stage, or until the heart rate returns to baseline or to a rate under 100 beats per minute.
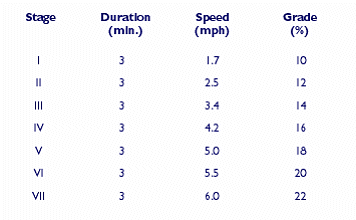
MULTISTAGE TREADMILL
EXERCISE PROTOCOL (Bruce)
Performance.
Following the resting ECG, the patient exercises at progressively increasing speeds and grades. For patients undergoing exercise testing, a predicted maximal achievable heart rate (PMHR) is calculated (220 minus the patient’s age). The patient’s peak achieved heart rate can be expressed as a percentage of the PMHR, giving an assessment of the adequacy of the test in stressing the heart. Studies have shown that if a patient achieves 85% or greater of his or her PMHR without developing signs of ischemia, the likelihood that significant CAD is present is reduced.
If a patient fails to reach 85% PMHR at peak exercise, CAD may be present but undetected by the test. The lower the peak rate (relative to the PMHR), the more likely that CAD, if present, will be missed. In the past, many laboratories would stop the exercise test when a patient reached 85% PMHR, to give a margin of
safety to the test. Currently, most laboratories perform symptom-limited maximal exercise tests and encourage patients to reach their maximal exercise effort. This way, the symptoms that limit the patient’s exercise performance can be determined and the patient can perform his or her maximal work safely. Patients who fail to reach 85% PMHR are still at risk of having significant, but undetected, CAD.
The test is terminated when any of the following occur:
- Typical anginal-type chest pain
- 85% of predicted maximum heart rate is achieved
- Dizziness and/ or lightheadedness
- Shortness of breath or muscular fatigue such that the patient is unable to continue
- Arrhythmias
- ST-T changes
- Fall in blood pressure
Interpretation.
A normal ECG during an exercise test demonstrates the absence of ischemic ST-segment abnormalities. The duration of the QRS and ST intervals remains relatively unchanged. Peak exercise levels are usually attained when the patient achieves at least 85% PMHR for his or her age and sex.
One way of classifying patients subjected to stress electrocardiography is by the presence or absence of the symptom of chest pain. In the presence of pain, a positive stress ECG suggests, with a great deal of certainty, that the patient has CAD. Approximately 30% to 40% of patients with a positive stress ECG have angina. A negative test, however, does not rule out CAD. Depending on the patient’s risk-factor profile, other clinical findings, and the recurrence of pain, further evaluation may be required. In the absence of pain, a negative test is of more diagnostic value than a positive test. A negative test rules out significant CAD with great certainty, whereas a positive test requires further evaluation to reach a definitive diagnosis.
A positive exercise ECG is defined as
- 1 mm or more, flat or downsloping ST-segment depression or elevation lasting 0.08 second after the J point
- Upsloping ST-segment depression of 1.5 mm or more measured at 0.06 to 0.08 second from the J point
- 2 mm or more increase in the ST-segment abnormality in patients with a baseline ST-segment depression
- The ischemic ECG response to exercise can be seen during and/or following exercise. It may either precede or follow the development of chest pain and may even be seen in the
absence of pain.
Other findings that suggest an ischemic response to exercise but must be evaluated according to
the patient’s clinical condition are:
- Anginal-type chest pain in the absence of ST-segment changes
- Premature ventricular contractions noted prior to, during, or after exercise
- Development of ventricular tachycardia
- Development of conduction disturbances or supraventricular tachyarrhythmias
- T-wave abnormalities (inversion, pseudonormalization)
Premature beats that tend to disappear with exercise may also indicate significant underlying CAD. Although a positive exercise test correlates well with the presence of significant coronary artery obstruction—particularly if two or more vessels are involved, the ischemic ECG response to exercise is not specific for CAD. It may be seen in patients with other types of heart disease, such as left ventricular hypertrophy and/or aortic stenosis, which have decreased tolerance to an oxygen deficit. A positive response may also be seen occasionally in healthy people—notably women—whose arteriograms show normal coronary arteries.
Alternatives to treadmill testing Patients who are unable to exercise or who have abnormal baseline electrocardiograms are not good candidates for treadmill testing. The pharmacologic stress test uses medications which alter the coronary blood flow. Such medications include Dobutamine, IV Dipyridamole, Adenoscan, and Regadenoson.
CARDIAC STRESS TESTING: Pharmacologic Stress Agents
The Role of Pharmaceuticals in the Evaluation of Heart Disease
Inadequate flow to meet myocardial demands leads to myocardial ischemia.
With exercise stress testing, we evoke ischemia by increasing demand for blood. Arteries dilate in response to the demand for oxygen. Areas where plaque has stiffened the coronaries will not dilate, causing transient (temporary) ischemia.
Using medications which alter blood flow is an effective and safe means to the same end. It is important that patients follow the prep guidelines the day of the exam with respect to food and beverage intake, and in many cases, caffeine or chocolate consumption.
Patients suffering from COPD, emphysema, reactive airway disease (asthma), or who are taking certain medications must be evaluated for active wheezing prior to administration of any vasodilator.
Pharmacologic agents are formulated to bind temporarily to specific receptors in the inner arterial lining for the purpose of affecting heart rate and/or blood pressure (dilatation). There are Alpha and Beta Receptor sites which, when stimulated, raise or lower heart rate and blood pressure.
Theophylline and caffeine are nonselective competitive blockers of adenosine receptors, and should be avoided 12-24 hours prior to administration of adenosine.
IV DOBUTAMINE
Dobutamine is an effective alternative to exercise for patients with severe asthma or bronchospastic disease. IV Dobutamine initiates an increase in oxygen demand, indirectly resulting in coronary vasodilation. Dobutamine is classified as a Synthetic Sympathomimetic amine, a synthetic catecholamine with sympathomimetic activity.
Dobutamine stimulates Beta 1 and Beta 2 Adrenergic Receptors. It increases coronary blood flow by increasing cardiac contractility and heart rate with a mild increase in vasodilation.
Certain factors or conditions may interfere with a dobutamine stress test. These factors include, but are not limited to, the following:
– smoking or ingesting caffeine within three hours of the procedure
– beta-blocking medications may make it difficult to increase the heart rate
Dobutamine is administered according to patient weight, starting with a low concentration and increasing with every three-minute stage. Dobutamine stress tests may be safely administered to the asthmatic patient and is routinely used with echocardiography in patients who are unable to exercise on a treadmill.
An advantage to Dobutamine is that it has a short half-life. One drawback to Dobutamine from a nuclear medicine tech’s point of view is that the radiotracer may not be absorbed into myocardial tissue adequately, and persistent liver activity makes it difficult to obtain decent gated SPECT images.
- Good for use in the asthmatic patient
- Dose titrated at 5, 10, 20, 30, and 40 mcg/kg/min by infusion pump in 3 minute stages
- Monitor patient for changes in ECG, HR, BP
- Dobutamine accelerates heart rate, resulting in coronary vasodilation
- Radiotracer injected at peak HR*, or when symptomatic, continue infusion 1 more minute
- Recovery stage 5 minutes
- Esmolol (a beta blocker) is the antidote
* atropine may be used to bring HR to peak after stage 5 completed
IV DIPYRIDAMOLE (Persantine)
When Dipyridamole first came on the scene in the 1980’s, an oral suspension was being used for nuclear perfusion testing. The intravenous version of the drug quickly gained widespread acceptance to evaluate myocardial perfusion in patients unable to walk on a treadmill.
- NOTE: Persantine can cause bronchospasm in the asthmatic patient and MUST NOT be used!
- NPO 4 hours, 2 hours if diabetic
- Caffeine, decaf avoided 24 hours
- Xanthine derivatives avoided 36-48 hours
Dipyridamole induces coronary vasodilation by elevating interstitial adenosine concentration by inhibition of adenosine uptake in vascular endothelium and on red blood cell membranes.
Dosage and Administration Protocol: Calculate patient weight in kg x .57 mg/kg= dose in mg, not to exceed 60 mg.
Draw up in 60 cc syringe, then
dilute to 40 cc with 0.9% normal saline. The patient is prepped with 10 electrodes and baseline and serial electrocardiograms are taken each minute. Administer dose at rate of 10 cc per minute over 4 minutes, wait until minute 7, then inject radiopharmaceutical intravenously. The tracer must circulate a minimum of one to two minutes prior to reversing the drug with Aminophylline.
OPTIONAL: Handgrip, hand weights and arm movement, bicycle ergometer, walk on flat treadmill 1 mph for 1 minute post DIP infusion and 1 minute following tracer injection.
Wait 45 to 60 minutes when imaging Tc99m tracers, within 10 minutes when using Thallium-201.
IV ADENOSINE (Adenoscan)
Adenoscan is a vasodilator which has a very short half-life. Adenoscan dose is calculated according to patient weight and is administered slowly over a 4 to 5 minute infusion using a pump.
Side effects most often include flushing, chest discomfort, and mild dyspnea. Rarely, stomach upset resulting in vomiting may occur. Because Adenoscan has an effective half-life of 30 seconds, side effects usually resolve quickly when infusion is terminated and generally do not interfere with test results.
Adenosine is a natural purine. In the heart, adenosine causes coronary vascular smooth muscle relaxation, inhibits norepinephrine released from sympathetic nerve endings, reduces AV node conduction velocity, and has inotropic and chronotropic effects. Coronary arteriole peripheral vasodilation leads to a small increase in heart rate and a fall in systolic blood pressure. Side effects include flushing, chest pain, headache, dyspnea, nausea and dizziness. Plasma half-life is very short, and the side effects, although common (80%), are short lived and well tolerated. Adverse effects include atrioventricular conduction block, sinus node dysfunction and bronchospasm. Adenosine should not be used in patients who have heart block without pacemaker protection, in those with sick sinus syndrome, or in those with asthma.
Aminophylline or nitroglycerine should be on hand for any serious reactions. Recovery begins when infusion is terminated and is typically 5 minutes. Blood pressures are monitored and recorded every minute during infusion and continues for 5 minutes into recovery. A small amount of a caffeinated beverage quickly reverses headache, nausea or residual feelings of malaise during the recovery period.
- Not for use in the asthmatic patient due to exacerbation of bronchspasm.
- NPO 4 hrs – 2 hrs. if diabetic
- Caffeine and chocolate products avoided 24 hours prior to testing
- Dose: 140 mcg/kg/min by infusion pump over 4 minutes
- Half-life of less than 10 seconds
- Monitor patient for changes in ECG, HR, BP
- When half of adenosine infused, inject tracer into port over 5-10 sec., infuse remaining adenosine
IV LEXISCAN (Regadenoson)
is an A2A adenosine receptor agonist that is a coronary vasodilator. It produces maximal hyperemia quickly and maintains it for an optimal duration that is practical for radionuclide myocardial perfusion imaging.
Regadenoson has a 2-3 minute biological half-life, as compared with adenosine’s 30 second half life. Regadenoson stress protocols using a single bolus have been developed, obviating the need for an intravenous line. Regadenoson stress tests are not affected by the presence of beta blockers, as regadenoson vasodilates but does not stimulate beta adrenergic receptors.
Regadenoson is a selective A2A-adenosine receptor agonist used as a pharmacologic stress agent in myocardial perfusion imaging (MPI) studies. Regadenoson has been designed to be delivered as a rapid intravenous bolus needing no specialized pumps or accessories. No dose adjustment for body weight is required. Regadenoson (Lexiscan) selectively stimulates the the A2A-adenosine receptor resulting in coronary vasodilation.
Contraindications to Regadenoson include
- Heart block, second or third degree (type of abnormal heart rhythm) or
- Sinus node dysfunction (type of abnormal heart rhythm)—Should not use in these conditions unless patients have a pacemaker that works.
- Breathing problems or lung disease (e.g., asthma or COPD) or
- Ischemia or
- Low blood pressure (hypotension)—> Use with caution, as the drug may make these conditions worse
Patients may be tested seated upright in a chair and instructed to ‘march in place’ to lessen side-effects during Lexiscan infusion. Patients with a low baseline blood pressure should be tested recumbent on a gurney. The nuclear technologist or cardiac nurse administers the drug under the direct supervision of a physician in many clinics. A prefilled 5-cc syringe containing the Lexiscan is administered as a bolus (20-30 sec.), followed by a 5-cc saline flush. Immediately inject the radiotracer, followed by another 5-cc saline flush. The drug and the tracer should be completely injected and flushed by the 1.0 minute mark, so the Recovery phase may begin at that point.
Side effects most often reported are headache and stomach upset. Iv aminophylline may be given 2 minutes after radiotracer, or just have the patient get a cup of coffee or cola after the stress test. Imaging may be commenced 45 minutes post stress.
Side effects to Pharmacologic Vasodilation
Dipyridamole and Adenosine can sometimes increase heart rate as a result of secondary response to vasodilation plus decrease in BP. Patients may exhibit a spike in heart rate during infusion, not the usual response to Dipyridamole, but it may be an effect of mild allergic reaction. In my own experience, unless the patient is also complaining of chest tightening or pain, we have continued infusion while closely monitoring the patient for adverse effects.
It is normal to experience ‘flushing’, an overall sensation of warmth, an the effect of vasodilation of all arteries and veins simultaneously. Other symptoms to watch for include chest pain, nausea and vomiting, dizziness, headache, shortness of breath, and a drop in blood pressure. Adenoscan has such a short half-life that reversal is not needed, except in extreme cases of acute shortness of breath or vomiting. Patients with emphysema may experience acute chest tightening within seconds of infusion, and administration of the stress agent must be immediately aborted.
To lessen the severity of the side-effects experienced with agents such as Dipyridamole and Adenosine, a “walking” medicine stress test can help the patient who is able to walk flat on a 1.0 mph belt speed. Getting the large leg and arm muscles involved, with walking, isometric leg and arm exercises, handgrip or stressball squeezing, may help the patient focus on something other than the appearance of side effects and helps burn off the medicine a little faster.
IV Aminophylline as an Antidote to Vasodilation
Aminophylline is a vasoconstrictor, having the same action on the vessels as caffeine, negating or reversing the effects of pharmacologic stress agents. Intravenous Aminophylline must be ready to administer should the patient experience unpleasant side effects from vasodilation, particularly from Dipyridamole, Regadenoson, and in cases of extreme reaction, Adenoscan.
An initial infusion of 50-75 mg Aminophylline is injected over the course of 30 seconds to 1 minute IV. A second dose may be repeated 2 minutes later. In some laboratories, Aminophylline is routinely administered after tracer uptake is complete (2 min post injection) as a prophyllactic against delayed unpleasant side-effects. The aminophylline should not be administered prior to radiopharmaceutical injection, since the vasoconstrictive effects would render the exam invalid. Severe angina is treated with sublingual nitroglycerin.
- 5a: CV Disease
- 5b: Coronary Syndromes
- 5c: Atherosclerosis
- 5d: Myocardial Infarction
- 5e: Stress Testing
- 5f: Cardiac Medications
- 5g: Revascularization
- Lesson 5 REVIEW
DOWNLOAD THESE RESOURCES:
1. Current Methods of Pharmacologic Stress Testing and the Potential Advantages of New Agents