A Cellular Perspective: Electrophysiology of the Heart
Cardiac tissue is specialized to generate and transmit electrical impulses. Characteristics of the cell membrane and the concentrations of ionic solutions (electrolytes), within the cell and outside it, make the conduction of electrical impulses possible.
Electrical potential is the voltage difference that exists across the membranes of cells. The cell membrane potential is created by mechanisms resulting in an excess of negative ions inside the cell and an equal number of positive ions immediately outside the membrane. The resting cell is therefore said to be polarized, and the membrane potential is -70 to -90 mv.
Under certain conditions, sodium and potassium atoms tend to lose an electron and ionize. This leaves a balance of one extra positive charge inside the cell. Calcium atoms form ions bearing two positive charges.
SELECTIVE PERMEABILITY OF THE CELL MEMBRANE
The myocardial cell wall is a semipermeable membrane containing channels, pores through which specific ions or other water soluble molecules can cross. These channels selectively allow some substances to pass into and out of the cell. The sum of the positive charges has to be the same on each side of the membrane.
K+ can more readily exit and enter the cell than can
sodium ions (Na+). During the resting state the membrane is relatively permeable to potassium ions (K+). The K+ concentration within the resting (polarized) cell is about 35 times greater than the extracellular concentration, while the Na+ concentration outside the cell is many times greater than the intracellular concentration.
Within the cell, the excess of K+ ions is accompanied by a large number of non-diffusible negative organic molecules (mostly proteins). These heavy anions cannot pass across the membrane to enter the extracellular fluid and remain within the cell. Since the resting cell membrane is so much more permeable to K+ than to Na+, there is more potassium normally leaving the cell than sodium entering. The result is the net outward movement of positive K+ ions, and the membrane resting potential is said to be related to the concentration gradient of potassium across the membrane.
THE ACTION POTENTIAL
Permeability refers to the ability of a membrane channel to conduct ions once it is open. The stimulus that alters the gradient across the cell membrane may be electrical, mechanical, or chemical. When a resting myocardial cell is stimulated by an impulse from the cardiac conduction system, the permeability of the cell membrane to sodium is suddenly increased. This elicits a sequence of rapid changes in membrane potential lasting only thousandths of a second, then a return to the resting potential. This sequence of changes comprises the action potential, which occurs in two stages: depolarization and repolarization.
POLARIZATION, DEPOLARIZATION, REPOLARIZATION
Polarization (the resting membrane potential) is the resting state during which no electrical activity occurs in the heart. When a cardiac muscle cell is polarized, the inside of the cell is more negative than the outside because of the numbers and types of ions found inside the cell. The primary intracellular ions include K+ and several negatively charged ions (anions). During the resting state, K+ ions leak out of the cell, leaving the negatively charged ions inside the cell. The result is a negative charge inside the cell.
When the cardiac muscle cell is stimulated, the cell is said to depolarize. Deopolarization is not the same as contraction. Depolarization is an electrical event expected to result in contraction, a mechanical event.
The inside of the cell becomes more positive because of the entry of Na+ ions into the cell through Na+ membrane channels. Thus depolarization occurs because of the inward diffusion of Na+. Deopolarization proceeds from the innermost layer of the heart (endocardium) to the outermost layer (epicardium). On the ECG, the P wave represents atrial depolarization, and the QRS complex represents ventricular depolarization.
After the cell depolarizes, the diffusion of Na+ into the cell stops, K+ is allowed to diffuse out of the cell, leaving the anions (negatively charged ions) inside the cell. Thus repolarization occurs because of the outward diffusion of K+. The membrane potential of the cell returns to its negative resting level. This causes the contractile proteins to relax and separate. The cell can be stimulated again if another electrical impulse arrives at the cell membrane.
Repolarization proceeds from the epicardium to the endocardium. On the ECG, the ST segment represents early ventricular repolarization and the T wave represents ventricular repolarization.
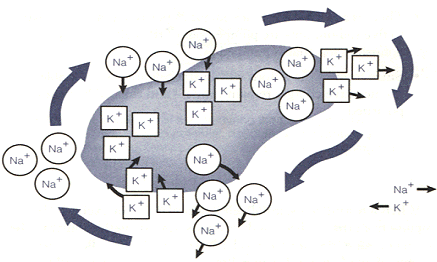
THE SODIUM-POTASSIUM PUMP, OR ACTIVE TRANSPORT
In the heart, the cardiac muscle cell membrane acts as a pump. Active transport describes the mechanism by which sodium ions are driven out of the cell faster than potassium ions are pulled in. This keeps cellular sodium levels low and potassium levels high. The unequal distribution of electrolytes between the intracellular and extracellular compartments is extremely important for the life and function of almost all cells, but it has particular importance in cells that transmit electrical impulses.
Sodium is transported outside the cell in combination with a carrier lipoprotein. On the outer surface of the membrane, the sodium is released, and the carrier combines with potassium and moves to the inner surface of the membrane. There, energy is provided by the breakdown of adenosine triphosphate (ATP) to split the potassium from its carrier. The carrier is then able to transport another sodium ion to the surface and thus continue the cycle. This pump requires a great deal of energy to function, since the ions are transported against their respective concentration gradients.
An excess of positive charges soon accumulates on the outside of the membrane. Suddenly, when the threshold is reached, the flow reverses. Ionic gates open in the membrane and sodium gushes back into the cell. This rapid shift in positive charges is called depolarization, and it creates an electrical current. Quickly the ions are pumped back out again, during the stage termed repolarization.
All electrical activity depends on a difference in potential. This unequal distribution of electrolytes is particularly important for the life and function of the myocardial cells because they transmit electrical impulses. If there were no such mechanism, passive diffusion over time would equalize concentrations of sodium and potassium inside and outside of the cell… yielding an equal potential.
ION DIFFUSION- PASSIVE TRANSPORT
The myocardial cell membrane is relatively impermeable to sodium when the cell is polarized- allowing some Sodium ions to pass from the high extracellular concentrations
to the lower intracellular concentrations. Because the membrane is relatively permeable, potassium can move to the outside as well as being transported to the inside. Thus, even in the resting cell there is some
movement of sodium and potassium in both directions.
PUTTING IT TOGETHER- THE CELL MEMBRANE POTENTIAL
- A sodium-potassium pump mechanism actively transports sodium to the outside and potassium to the inside.
- The resting cell membrane is much more permeable to potassium- perhaps 50-100 times as much- which allows potassium to diffuse through the membrane relatively easily while sodium diffuses with difficulty. This is a passive transport mechanism.
- Inside the cell are large numbers of heavy, negatively charged molecules that cannot normally diffuse through the membrane.
- There is a net outward movement of positive ions, since two to five sodium ions are pumped out of the cell for every potassium ion that is pumped in.
- Since most of the anions within the cell are nondiffusible, the negative charges remain inside- and the cell becomes polarized.